
ASHEBORO, N.C. (ACME NEWS) — A $319 million funding gap could cut off more than 3 million North Carolinians from Medicaid coverage as soon as this month, state officials warn.
North Carolina’s Medicaid program has been underfunded since last year, when the state legislature fell $319 million short of what the program needs to operate through the end of the fiscal year. That gap has lingered for months as lawmakers failed to reach a final agreement or pass a state budget. With the legislature set to return April 21, state health officials say time is running out for millions of people who depend on the program.
What is Medicaid, and who does it cover?
Medicaid is a government health insurance program for people with lower incomes, funded jointly by states and the federal government. In North Carolina, the federal government covered about 73% of the program’s costs last year — roughly $14 billion of a $19.4 billion total — with the state paying the rest.
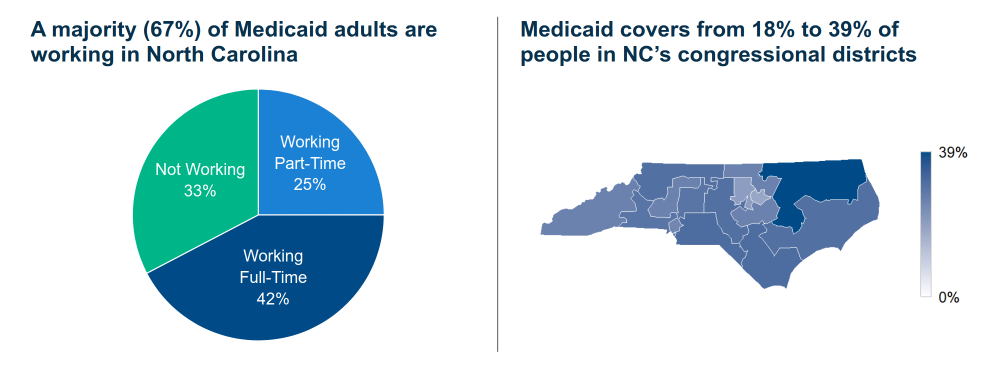
The program covers about 1 in 4 North Carolinians, including children, pregnant women, elderly residents, people with disabilities and working adults. It pays for half of all births in the state, covers 61% of nursing home residents and insures two in five children — with even higher rates in rural communities. Most adult Medicaid enrollees in North Carolina are working. About 42% work full-time and another 25% work part-time, according to 2025 data from KFF, a nonprofit health policy organization.
North Carolina expanded Medicaid in December 2023 under the Affordable Care Act, extending eligibility to adults ages 19 through 64 earning up to 138% of the federal poverty level. More than 600,000 residents became newly eligible, and about 300,000 were automatically enrolled on the first day.
How did the program end up short?
Health care costs have been on the rise, and Medicaid is not immune. Inflation, expensive new medications, growing demand for mental health and autism services, and new federal requirements have all driven up costs.
The North Carolina Department of Health and Human Services (DHHS), which runs Medicaid in N.C., asked the General Assembly — the state legislature — for $819 million in additional funding last year to keep up with those rising costs. Lawmakers provided only $600 million, leaving a $319 million gap.
DHHS first notified lawmakers of the funding problem in May 2025. Both the House and Senate introduced proposals to fully fund Medicaid, but the two chambers could not reach agreement before adjourning in late October — returning only briefly for a redistricting session before leaving town for the year.
A special session called by Gov. Stein in November also failed to break the deadlock — leaving North Carolina as the only state in the country without an enacted budget; and its Medicaid program still $319 million short.
With no additional funding in place, DHHS took steps to reduce the rates it pays to doctors, hospitals and other health care providers by 3-10% in Oct 2025. The cuts were intended to slow spending and keep the program solvent while lawmakers worked toward a solution.
However, in Dec 2025, court rulings struck down those cuts forcing Gov. Josh Stein to direct DHHS to restore the rates to normal. In a letter to providers, DHHS warned that without the rate cuts as a management tool, it now had “no remaining mechanisms” to responsibly manage the shortfall — making the financial situation more precarious.
Medicaid is currently underfunded by $319 million. With the rate reductions no longer an available tool at this time, NCDHHS now has no remaining mechanisms to responsibly manage this funding gap. As a result, the Medicaid program is projected to run out of money early next year.
If this happens, the consequences will be far more severe than the rate change. The stability of the entire Medicaid program – and the care provided to more than three million North Carolinians – is at risk.
What happens if lawmakers don’t act?
DHHS officials told state lawmakers in late March that without additional funding, Medicaid is expected to run out of money sometime in April — before the fiscal year ends June 30.
“There will come a point where we may have a couple hundred million dollars, but we don’t have enough to pay all of our health plans or we don’t have enough to pay all of our vendors,” Melanie Bush, DHHS’ interim assistant secretary for Medicaid, told the Joint Legislative Oversight Committee on Medicaid.
If coverage is disrupted, people who rely on Medicaid for regular prescriptions, mental health appointments, disability services, home health aides and nursing home care would be most immediately affected.
What comes next?
The General Assembly is scheduled to return April 21 for its short legislative session. Medicaid funding is expected to be among the first items taken up. Gov. Stein has requested $319 million as part of a broader $1.4 billion emergency budget package.
Some Republican lawmakers have expressed skepticism about the size of the request and have said they want to examine why Medicaid costs keep rising before committing to long-term funding increases.
The two largest cost drivers, according to DHHS, are services for older adults and people with disabilities — a group that makes up about 23% of enrollees but accounts for 64% of total spending — and the growing use of autism-related therapies.
For now, if you are on Medicaid, your coverage has not been cut. But state health officials say that could change quickly if the legislature does not act before the program’s funds run out.
Lawmakers Sen Jim Burgin (R), Sen Dave Craven (R), and Rep Carla Cunningham (D) did not respond to Acme News’ requests for comment on the budget shortfall prior to publication.
###

